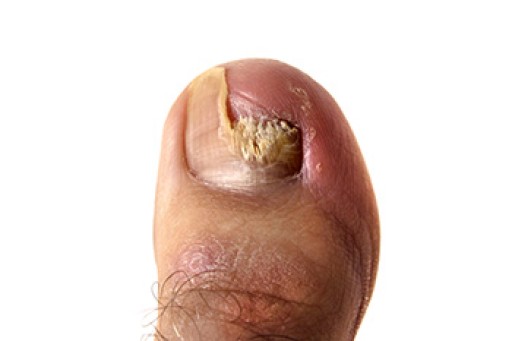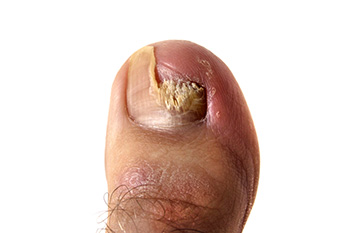
Onychomycosis is a fungal infection that affects the toenails, often leading to brittle, discolored, and thickened nails. Common symptoms include yellow or white streaks under the nail, a distorted nail shape, and, in severe cases, pain or discomfort. This infection can also cause nails to crumble or separate from the nail bed, making it not only unsightly but also potentially painful. Effective treatments for onychomycosis vary depending on the severity of the infection. Topical antifungal medications are often prescribed for mild cases, while more persistent infections may require oral antifungal medications. In some situations, nail debridement or laser therapy might be recommended to promote healing and restore nail appearance. Maintaining good foot hygiene and avoiding damp environments can help prevent recurrence. If you suspect you have onychomycosis or are struggling with toenail issues, it is suggested you schedule an appointment with a podiatrist. This type of doctor can provide a proper diagnosis and tailored treatment plan to help restore healthy toenails.
For more information about treatment, contact one of our podiatrists of Lewis Wolstein, DPM, P.C. & Associates. Our doctors can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please contact our office located in Co-Op City, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.